Future Trends in Laparoscopic, Robotic Surgery Tools and Trocar Site Management
- sutureease
- Mar 12
- 5 min read
The headlines around laparoscopic, robotic surgery tools tend to focus on consoles, instrumentation, and data. But the last minutes of a case still carry outsized impact: trocar site management.
For surgeons, the key to a clean finish to a procedure is securing a closure they can trust. For hospital teams, it’s a controllable step that can influence downstream utilization, including follow-up visits and hernia repair pathways.
Below is a practical way to think about where tools are going and why fascial closure workflow is still a key variable.
“Intelligent” Robotics Is Shifting Expectations in the OR
Next-generation laparoscopic, robotic surgery tools are increasingly defined by sensing and guidance rather than pure mechanical dexterity. Three themes are showing up across platforms and instrument roadmaps:
Haptic feedback and tissue sensing: Systems are working to restore “feel” through sensors that interpret resistance and translate it to the surgeon’s console. That matters for delicate tissue handling and for consistent suturing behavior.
Workflow assistance: AI features are being built to recognize steps, reduce friction between phases of the procedure, and flag potential risks. Whether or not every feature delivers measurable time savings, the direction is clear: fewer “guesswork” moments.
Miniaturization and access evolution: Smaller instruments and more concentrated access (including single-port concepts) raise the bar for what “minimal access” means, especially when closing defects reliably becomes harder, not easier, as working space tightens.
The implication: as front-end technology becomes more guided and more standardized, the back-end steps (including port closure) can’t remain inconsistent.
Trocar Site Management Remains a Persistent Challenge
Even with smaller incisions and better visualization during the case, trocar site issues (particularly trocar site hernias or TSH) remain clinically relevant. Clinical literature (1-4) cites an incidence range of 1–8% with published findings showing higher hernia rates at 12 mm port sites when fascia is left open (8%) versus closed (0.22%) in gynecologic laparoscopy.
Most teams already know the rule of thumb: close ports ≥10 mm. The challenge is making that closure reproducible across patient types, port locations, and staffing patterns. Current best-practice direction tends to cluster around three needs:
Standardization With Risk Awareness
There is broad consensus to close fascia at ports ≥10 mm because of increased herniation risk. Where protocols are evolving is in recognizing when closure is “technically harder than it sounds” (for example, higher BMI, diabetes, and age) without letting those factors become a reason to avoid closure altogether and take the risk.
Closing the “Depth Gap” in High-BMI Patients
As the distance from skin to fascia increases, hand suturing becomes slower and less predictable. This is one reason extended-reach closure options remain relevant even as instruments get smaller.
Under-Vision Closure Over Blind Passes
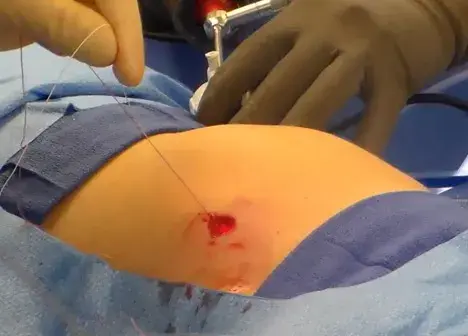
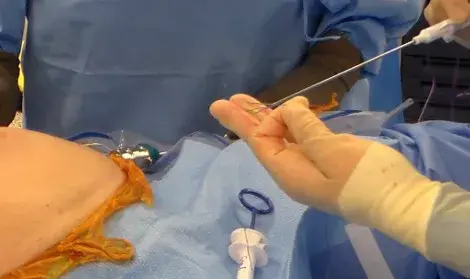
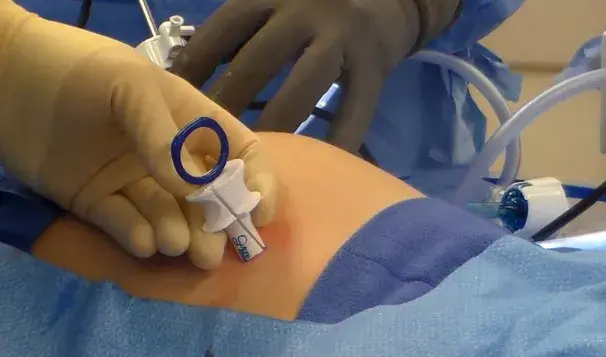
Workflows that support closure under laparoscopic vision reduce uncertainty: you can confirm that the needle path captures fascia/peritoneum appropriately and avoid unintended injury during instrument passage. The SecurusDL Study (Suture Ease, Galt, CA) describes a technique performed under direct laparoscopic vision, with repeatable stitch placement and symmetric bites.
Where Suture Ease Fits: Simple, Repeatable Closure Inside a Modern Workflow
There’s a counter-pressure in the OR: as platforms become more complex, teams still want closure tools that reduce steps, reduce variability, and fit training realities.
Suture Ease positions CrossBow™ and LongBow™ as a patient-tailored approach; the closure method can adapt to the patient tissue quality and access situation, rather than forcing one device with no adjustability.
Crossbow™: Guided Capture With Snare-Loop Retrieval
CrossBow is built around a guide-and-snare workflow intended to reduce “fishing for suture” and to support consistent capture and retrieval. Suture Ease’s predecessor device (SecurusDL) used the same snare-loop concept and, in a multi-patient evaluation, recorded a mean closure time of 67 seconds (range 45–96) with uniform, symmetric stitch placement observed across cases.
Longbow™: Extended Reach for Deeper Abdominal Walls
LongBow addresses the same closure objective (secure fascial defect closure) while accounting for increased depth in higher-BMI patients, where access and angle can compromise consistency.
Adjustable Fascial Bite: Matching Closure to Tissue Quality
Clinical literature (6-7) also cites why bite size matters: studies in open procedures have linked larger fascial bites with higher pain scores, while poor tissue quality may require a larger bite to reduce suture tear-through risk. CrossBow includes guide indicators to adjust bite placement relative to fascia/peritoneum to help tailor closure to tissue quality.
Trocar Site Closure Workflow: What Changes When You Use a Guided System?
This table shows how trocar site closure workflow changes when you move from manual closure to a guided system. The goal is more repeatable fascial capture and suture retrieval, especially at ≥10 mm ports and in deeper abdominal walls.
Closure Goal | Manual Hand Suturing | Guided Snare-loop Closure (Guide-assisted) |
|---|---|---|
Fascial capture consistency | Varies by angle, depth, assistant support | Designed to support repeatable placement under vision |
Steps prone to delays | Finding/holding suture ends, repeated passes | Snare-loop retrieval reduces manual retrieval steps |
High-BMI practicality | Depth increases difficulty and variability | Extended reach option (LongBow) supports deeper access |
Bite control | Often dependent on feel and exposure | Guide indicators support adjustable bite concept |
Future Outlook: “No-Trace” Expectations and Value-Based Pressure
The direction of travel is clear: minimally invasive surgery is being judged more on the recovery curve, not just the intraoperative result. For hospital decision-makers, the financial side isn’t abstract; TSH often requires surgical intervention, and preventing avoidable complications supports quality metrics and resource control.
For surgeons, the practical question is simpler: does the closure step stay consistent when the case is long, the patient is high-BMI, and the port site is awkward? Tools that support under-vision closure, consistent capture, and controllable bite size are aligned with where laparoscopic, robotic surgery tools are heading overall: more standard work, fewer variable outcomes.
If you’re looking at how trocar site management fits into your laparoscopic and robotic workflow, contact us for more information and discuss whether CrossBow™ or LongBow™ aligns with your standard closure protocol.
References:
1. A Soroush 1, Z Khorgami 1*, Y Jahangiri 1, R Mofid 1, S Nasiri 1, A Aminian, A Alibakhshi. Assessing Effect of Fascial Non-Closure in 10 mm Trocar Sites on Incidence of Incisional Hernia. J Minim Invasive Surg Sci.2013;2(1): 99-102
2. Shaher Z. Port closure techniques. Surg Endosc. Aug 2007;21(8):1264-1274.
3. Swank HA, Mulder IM, la Chapelle CF, Reitsma JB, Lange JF, Bemelman WA. Systematic review of trocar-site hernia. Br J Surg. Mar 2012;99(3):315-323.
4. Kadar, N., Reich, H., Liu, C. Y., Manko, G. F. & Gimpelson, R. Incisional hernias after major laparoscopic gynecologic procedures. Am. J. Obstet. Gynecol. 168, 1493–1495 (1993).
5. Helgstrand F, Rosenberg J, Bisgaard T. Trocar site hernia after laparoscopic surgery: a qualitative systematic review. Hernia. Apr 2011;15(2):113-121.
6. Ghai GS, S H. A Comparison of a Small-Stitch Closure With a Standard Closure in Midline Laparotomy Incisions: A Prospective Comparative Study. Cureus. 2023 Dec 6;15(12):e50035. doi: 10.7759/cureus.50035. PMID: 38186468; PMCID: PMC10768337.
7. Millbourn D, Cengiz Y, Israelsson LA. Effect of stitch length on wound complications after closure of midline incisions: a randomized controlled trial. Arch Surg. 2009 Nov;144(11):1056-9. doi: 10.1001/archsurg.2009.189. PMID: 19917943.

Comments