How Ergonomic Laparoscopic Instruments Improve Workflow in the O.R.
- sutureease
- Mar 24
- 4 min read
When people talk about “the future” of minimally invasive surgery, the conversation often centers on robotic platforms and visualization. But laparoscopic instruments still do a huge amount of the work, especially in high-volume service lines where efficiency and repeatability matter.
For surgeons, handheld ergonomics affect fine control at the tissue level. For materials and perioperative teams, they affect consistency, turnover, and how reliably a standard closure step gets done at the end of the case.
Ergonomics has always been about reducing friction in the workflow, so the surgeon can execute the same sequence, the same way, case after case.
The Hidden Cost of Non-Ergonomic Laparoscopic Instruments
Laparoscopy creates a unique physical setup: the surgeon’s hands are operating through a fixed pivot point at the abdominal wall, while the eyes are locked on a screen. That “hands here, eyes there” alignment increases physical strain and mental demand even before you factor in a handle that doesn’t fit the user.
Common signs your laparoscopic instruments are working against you:
Non-neutral posture: elevated shoulders, neck rotation, wrist extension, and sustained grip
Extra “micro-adjustments”: repeated re-gripping, resetting the angle, or re-centering the tip
More mental bandwidth spent on the tool: when actuation feels stiff or inconsistent, attention shifts from tissue handling to instrument management
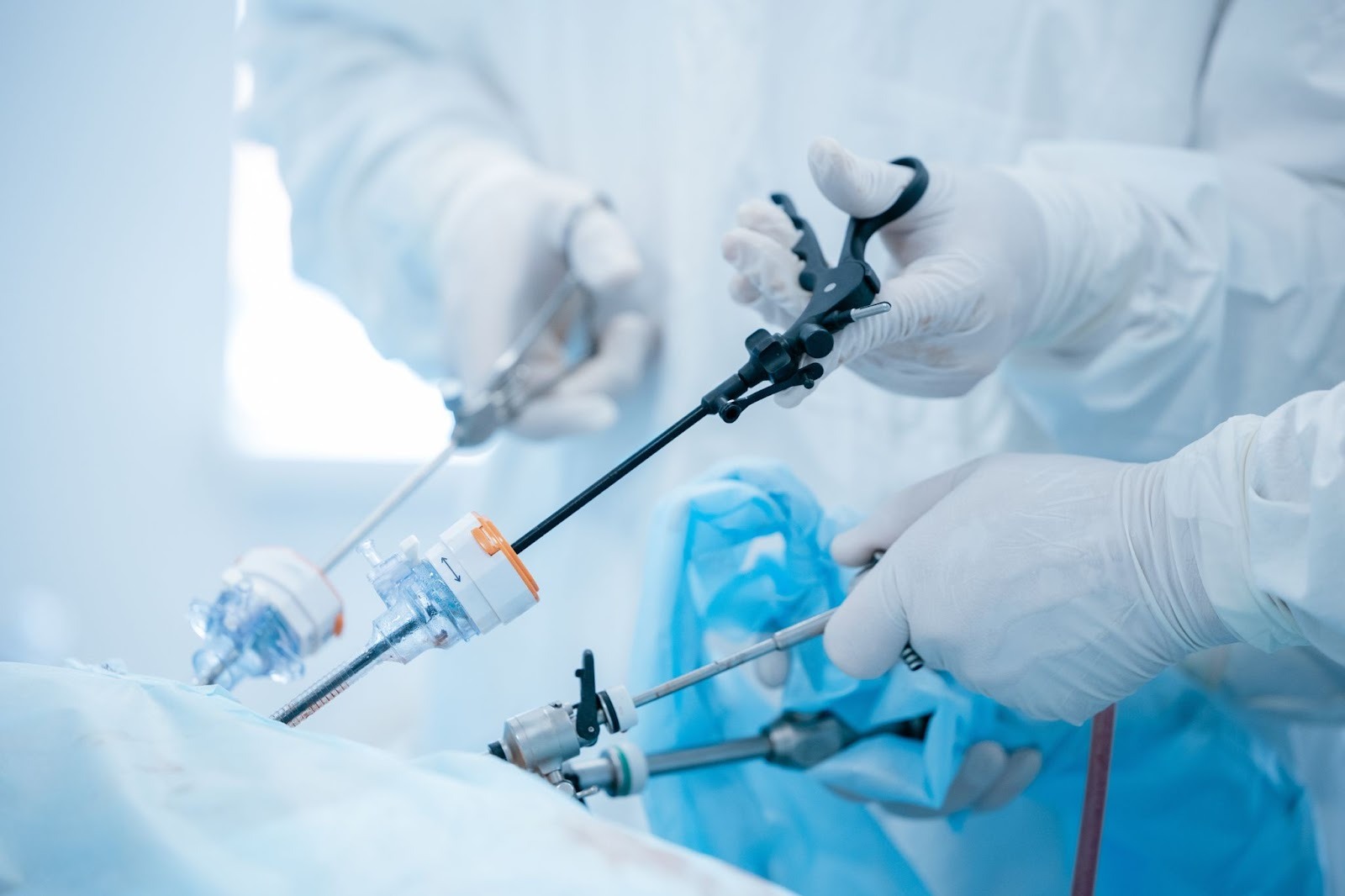
The last steps of the case make this more obvious. Trocar site management is often performed when the team is already deep into a procedure and fatigue is real. Closure tools that demand multiple hand changes or awkward wrist positions can turn a routine step into a slow one.
How Ergonomic Laparoscopic Instruments Remove Workflow Friction
Ergonomics is “fit the task to the person,” and in the O.R. that translates to steadier control and fewer unnecessary motions. Three design elements matter most.
1) Balance That Supports Precision
A well-balanced instrument helps the surgeon hold a stable position without fighting tip-heaviness. That matters during closure steps where the needle path needs to be controlled and repeatable; small deviations can lead to shallow bites, inconsistent capture, or more than one attempt.
2) Intuitive Actuation That Reduces Grip Stress
Instruments that require high grip force tend to increase fatigue and lead to compensations: changing hand position, shifting posture, or squeezing harder than necessary. Ergonomic actuation aims for a motion that’s natural and consistent.
In fascial closure, the “fumble factor” often comes from the capture-and-retrieval sequence: if the surgeon has to hunt for suture, switch grips, or make repeated passes, the step becomes less predictable. A guided capture workflow can simplify this into a more continuous motion rather than a series of recoveries.
3) Under-Vision Closure and Predictable Needle Control
The direction in trocar site closure is away from blind hand passes and toward workflows that keep control of the needle path. When the surgeon can confirm positioning and capture, it reduces uncertainty and supports consistent execution, especially in deeper abdominal walls where angle and reach become limiting factors.
Where Crossbow™ and Longbow™ Fit in an Ergonomic Closure Workflow
Suture Ease’s CrossBow™ and LongBow™ fascial closure systems are designed around a simple idea: at the end of a minimally invasive case, the closure step should be controlled, repeatable, and easy to teach.
CrossBow™ uses a guide and snare-loop concept intended to reduce manual suture retrieval steps and support consistent capture and retrieval. In practical terms, that means fewer “search” motions and fewer resets.
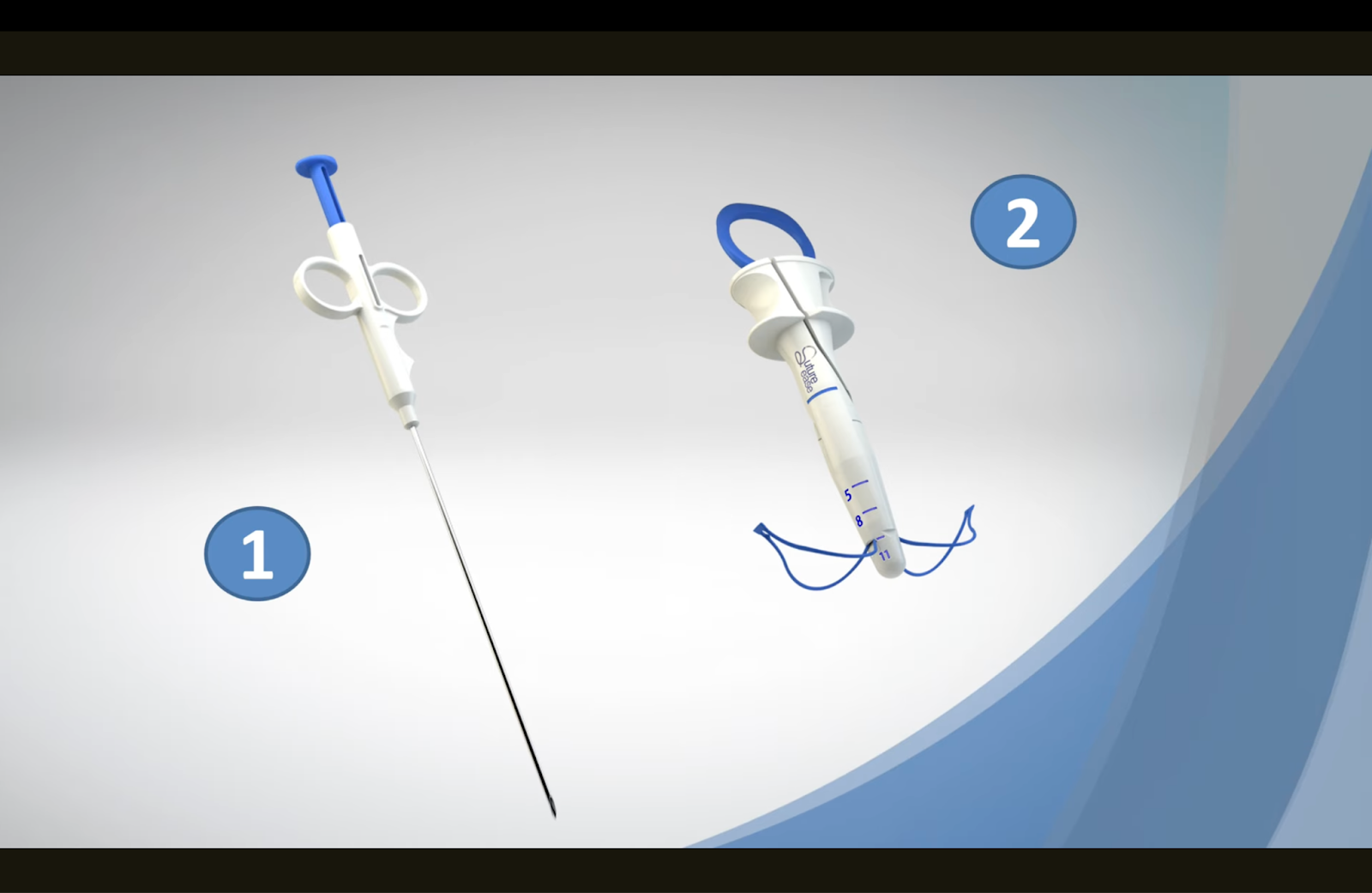
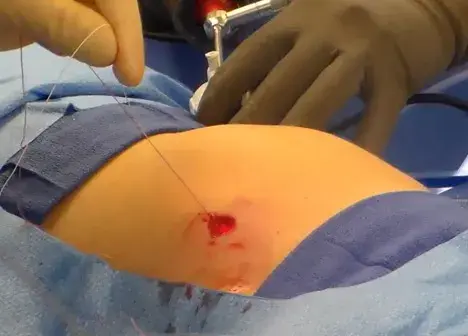
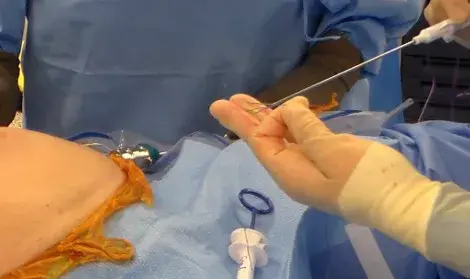
LongBow™ extends that same workflow for cases where tissue depth makes standard closure harder, commonly seen in bariatric and high-BMI patients. Extended reach isn’t just about length; it’s about maintaining a stable angle and controlled handling when the fascia is farther from the skin surface.
Adjustable bite capability also matters. Tissue quality varies. A closure approach that supports choosing a smaller adequate bite when appropriate (and a larger bite when tissue quality calls for it) helps teams standardize technique without forcing a single bite strategy on every patient type.
Why Materials and Perioperative Leaders Should Care
Ergonomic laparoscopic instruments are not “nice-to-have” items when you look at system impact. They can influence several operational outcomes that hospital teams track.
O.R. flow and turnover: When closure is more predictable, the end-of-case cadence tends to tighten. Fewer re-attempts and fewer hand-offs reduce small delays that stack up over a day of cases.
Training and standard work: Instruments that feel intuitive are easier to onboard across surgeons, first assists, and residents. That supports a standardized approach to trocar site management rather than a collection of personal workarounds.
Surgeon longevity and staffing stability: Physical strain is a real factor in surgeon satisfaction and endurance. Tools that reduce unnecessary force and awkward posture support sustainable performance, especially in long lists and complex cases.
A Quick Evaluation Checklist for Ergonomic Laparoscopic Instruments
Use this as a simple, shared framework between surgeons and materials teams:
Evaluation area | What to look for | Why it matters |
|---|---|---|
Handle fit and control | Natural wrist position, stable grip, minimal hand strain | Reduces compensations and fatigue |
Actuation effort | Smooth mechanism, consistent response | Supports control and repeatability |
Balance | No “tipping” at the distal end | Helps steady positioning in fine tasks |
Closure workflow | Fewer steps, less manual retrieval, controlled needle path | Reduces re-attempts and variability |
Reach options | Standard + extended-length availability | Helps match tool to patient depth |
Perform Surgeries More Efficiently With Suture Ease
The best O.R. workflow is the one you can repeat without fighting your tools. Ergonomic laparoscopic instruments support that repeatability by reducing unnecessary movements, lowering physical strain, and keeping attention on the tissue.
As minimally invasive programs expand into more complex patient populations, trocar site management becomes an even more important “last mile” step. Tools like Suture Ease’s CrossBow™ and LongBow™ are built to make that final step controlled and consistent, so “minimally invasive” doesn’t end with an avoidable closure problem.
Contact us for more information about CrossBow™ and LongBow™ and how they can fit into your trocar site closure workflow.

Comments